The processes underlying the transformation of sound into neural signals are poorly understood, and the temporal and spatial resolution of most in-vivo imaging modalities are insufficient to advance progress in this area. But optical coherence tomography (OCT) has recently emerged as a promising solution.
ByHrebesh M. Subhash and Alfred L. Nuttall
The complex inner ear structure called the cochlea is responsible for auditory transduction, which is the process of transforming the mechanical vibrations of sound into neural signals that are sent to the brain. The physiological processes underlying this transformation are poorly understood. In clinical otolaryngology, a number of non-optical in-vivo modalities—such as computed tomography (CT), magnetic resonance imaging (MRI) and ultrasound—have enabled visualization of the functionality and micro-anatomical features of the inner ear, but none has sufficient temporal and spatial resolution to help scientists research the micro-anatomy and functional dynamics of cochlear micro structures.
Recent technical developments in optical coherence tomography (OCT)—including advances in optical sources for high-resolution imaging, fast scanning methods, Doppler and other functional imaging features, and digital acquisition and image processing—have helped shed light a range of clinical imaging fields, such as dermatology, gastroenterology, intravascular imaging and otolaryngology. OCT’s high-resolution, real-time, minimally/noninvasive volumetric imaging capabilities make it ideally suited, too, for monitoring intra-cochlear structures with high resolution and sensitivity. Recently, a team of researchers at Oregon Health and Science University (Portland, OR) has developed a high-speed Fourier-domain OCT (FD-OCT) system specifically for this application, and has applied it in mouse and guinea pig models.
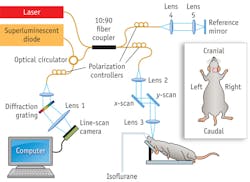
In the experimental setup, light from a 56 nm bandwidth low-coherence broadband infrared superluminescent diode light source (1300 ± 28 nm) is split into two paths in a 10:90 fiber-based Michelson interferometer (see Fig. 1). One beam is coupled onto a stationary reference mirror and the second is focused and scanned using a pair of galvo mirrors. The light emerging at the output of the interferometer is sent to a custom-built, high-speed spectrometer. The spectrometer consists of a transmission grating (1175 lines/mm), a camera lens with a focal length of 100 mm, and a 1024 element line-scan infrared InGaAs detector with a 25 µm pixel pitch size. The spectral resolution of the designed spectrometer is approximately 0.141 mm, which provides a total depth range of ~3.0 mm in air (2.22 mm in biological tissue, assuming the refractive index of the sample is ~1.35 mm). The axial resolution of the system is 13 µm in air (~9.6 µm in tissue). Our research team uses an objective lens with a focal length of 50 mm to deliver the probe beam onto the sample, providing a transverse resolution of ~16 µm and imaging depth of ~2.45 mm.
Intra-cochlear microstructural imaging
In-vivo imaging of inner ear microstructures is critical for understanding the pathophysiology of several inner ear disorders. High-resolution visualization of intra-cochlear micro structures such as Reissner’s membrane, organ of Corti, and basilar membrane could reveal morphological changes associated with various inner ear disorders—including Meniere’s syndrome, sudden and subacute sensorineural hearing loss (SNHL), the presence of a perilymphatic fistula, and certain autoimmune inner ear diseases—and could improve the ability to diagnose and comprehend these poorly understood conditions. To demonstrate the feasibility of FD-OCT for this purpose, we tried a mouse model. Using sterile surgical techniques, we used a ventral incision approach to access the cochlea, and generated various 3-D volumetric views based on segmentation of OCT data in the sagittal and coronal planes. The images clearly reveal various micro-morphological structures such as otic capsule, modiolus, Reissner’s membrane, basilar membrane, scala tympani, scala media, organ of Corti and scala vestibuli (see Fig. 2).
Intra-cochlear microvascular perfusion imaging
Along the same lines, detailed knowledge of cochlear vascular anatomy and perfusion is essential for understanding not only the function of hearing, but also the pathophysiology of otologic disorders such as noise-induced hearing loss, endolymphatic hydrops and presbycusis—which are thought to involve an abnormal regulation of cochlear blood flow (CoBF).
Normal blood supply to the cochlea is critical to generating the ionic concentrations required for auditory transduction, the mechanism by which sound waves are converted to nerve impulses that are carried by the eighth nerve and auditory pathway to the cortex. We know that the cochlear lateral wall receives its blood supply from a tight network of extremely slender vessels emanating from the central core of the cochlea (modiolus). Further understanding of the relation between the dynamics of cochlear blood flow and hearing function would help to improve diagnosis and treatment of SNHL that potentially arises from circulatory abnormalities. However, it has been difficult to find direct evidence of CoBF impairment in various kinds of sensorineural hearing loss. This is largely because there is currently no effective imaging tool available to directly observe the blood flow and vasculature within the cochlea that is surrounded by bone (otic capsule).
Thankfully, OCT has proven to be a powerful tool for mapping depth-resolved microvascular perfusion with high sensitivity and resolution. We have developed a variant OCT modality for extracting microvascular perfusion with ultra-high sensitivity called ultra-high sensitive optical microangiography (UHS-OMAG). The flow sensitivity of our imaging technique is high enough for extracting the slow capillary flows as low as 4 µm/s within the intact cochlea. An en-face (x-y) projection view of the perfusion through the vascular network located in the upper surface of the mouse cochlea clearly provides the visualization of depth-resolved microvascular map of cochlea (see Fig. 3).
In 3-D volumetric reconstructions of the microvascular perfusion in the cochlea, it is clear to see that the arterial blood supply to the lateral wall is emanating from the modiolus, which also contains the cochlear nerve, but is not visible in these images (see Fig. 4).
Imaging high sensitive vibrations of intra-cochlear membranes
In the cochlear mechanics research community, there is a great interest in studying the acoustic-induced vibrations of various membranes in the complex structure of cochlea, which is essential for understanding the cochlear mechanics and how the traveling wave of the basilar membrane couples its energy to the mechanosensory receptor cells in the spiral-shaped organ of Corti. To address this need, we implemented a novel, phase-sensitive spectral-domain OCT (PS SD-OCT) imaging modality to characterize intra-cochlear membrane vibrations at subnanometer scale. In order to test the feasibility of the PS SD-OCT system to image the high sensitive vibration of organ of Corti, we imaged an excised guinea pig cochlea at the apical end. We stimulated the cochlea using sounds at 100, 200, 300, 400, and 500 Hz frequencies.
Using this approach, we were able to visualize multiple turns of the cochlea, and clearly see the effect of vibrations from the Reissner’s membrane, reticular lamina, and basilar membrane (see Fig. 5). A vibrating flap, leftover from the opening created on the bony wall of the apical turn, was visible, and it became evident that vibration signal is obtained only from the location of the organ of Corti and not from the bony areas. We are able to get signals from various turns of the cochlea—which have different frequency responses—and thus are potentially able to study the response of a large region of the cochlea at the same time. This capability is currently not possible with any other technique.
ACKNOWLEDGEMENTS
The author acknowledges the contribution of Dr. Alfred L. Nuttall, Dr. Niloy Choudhury, Dr. Fangyi Chen, Dr. Ruikang K. Wang, and Dr. Steven L. Jacques.
REFERENCES
1. H.M. Subhash et al., IEEE Trans. Med. Imaging, 30 (2), 224–230 (2011).
2. H.M. Subhash et al., J. Biomed. Opt. 15, 036024 (2010).
3. N. Choudhury et al., Proc. SPIE 7889, 788930 (2011).
Hrebesh M. Subhash is a scientist with the Biophotonics and Functional Imaging Lab at Oregon Health and Science University (OHSU) in Portland, OR, and Alfred L. Nuttall is Director at the Oregon Hearing Research Center at OHSU; www.ohsu.edu/xd/. Dr. Hrebesh may be contacted at [email protected].
More BioOptics World Current Issue Articles
More BioOptics World Archives Issue Articles