OCT quantifies gas-assisted laser surgery outcomes
In the same manner that gas-assisted laser machining reduces flare-ups in flammable materials and clears debris for improved cutting and ablation, it is surmised that gas-assisted laser surgery could reduce soft-tissue surface heating and increase etch rates for hard-tissue ablation. In an attempt to better understand these beneficial processes as well as potential negative effects such as carbonization/charring and/or deformation of biological tissue, researchers at Ryerson University, the University of Toronto, and Sunnybrook Health Sciences Centre (all in Toronto, ON, Canada) used optical coherence tomography (OCT) to quantify one surgical example: in situ spinal-cord deformation/deflection as a function of various nitrogen gas-jet flow rates.
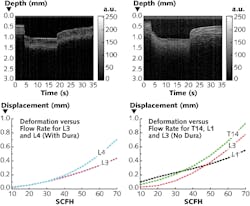
During laminectomy processes on pig spinal cords with both intact and removed spinal-cord dura, two aiming lasers and the flow nozzle output converged at the sample for OCT imaging. The images were background-subtracted, speckle was removed with a median filter, and a threshold filter identified edge positions for the acquired data. The OCT system observed spinal-deflection values ranging from 0.02 to 0.5 mm with the dura intact and 0.02 to 0.9 mm without it (see figure; also shown are two example OCT scans); a flow rate of 30 standard cubic feet per hour was the threshold for significant change in flow rate for both cases. Without the dura, mechanical noise due to vibrations induced by the gas jet reduces depth penetration of the OCT measurement; future work will focus on spinal-cord elasticity and how gas flow could improve surgical outcomes and even OCT-assisted surgical precision. Reference: R. Wong et al., Biomed. Opt. Express, 6, 1, 43–53 (Dec. 5, 2014).
About the Author

Gail Overton
Senior Editor (2004-2020)
Gail has more than 30 years of engineering, marketing, product management, and editorial experience in the photonics and optical communications industry. Before joining the staff at Laser Focus World in 2004, she held many product management and product marketing roles in the fiber-optics industry, most notably at Hughes (El Segundo, CA), GTE Labs (Waltham, MA), Corning (Corning, NY), Photon Kinetics (Beaverton, OR), and Newport Corporation (Irvine, CA). During her marketing career, Gail published articles in WDM Solutions and Sensors magazine and traveled internationally to conduct product and sales training. Gail received her BS degree in physics, with an emphasis in optics, from San Diego State University in San Diego, CA in May 1986.