Small probe takes OCT deep into the body
A research team at the University of California-Irvine (UCI; Irvine, CA) is using a five-year, $2.9 million National Institutes of Health grant to develop a microscopic probe for detecting and treating precancerous and malignant tumors in humans. The camera-equipped probe would enable doctors to look for microscopic abnormalities inside the gastrointestinal system. The researchers believe the probe could become a noninvasive substitute for conventional tissue biopsies that provides earlier detection of abnormalities; they plan to begin testing the probe in pigs and human volunteers to determine its effectiveness and safety.
The probe would be inserted into a patient and then guided through the esophagus, stomach, and colon to determine whether tumors are growing on the wall of the intestine. A surgeon operating an endoscope will remotely control the probe. The broadband (supercontinuum) light source will be a photonic-crystal fiber.
"Currently, gastrointestinal cancers and other diseases are diagnosed only by visual inspection of the intestine's surface," said Dr. Kenneth Chang, director of the H.H. Chao Comprehensive Digestive Disease Center at UCI. "Early-stage cancer screening is difficult because you're looking for microscopic changes. An optical probe could help pinpoint those changes before they turn into advanced cancer. It also may allow physicians to circumvent traditional biopsies that require removing tissues by providing an optical, or virtual, biopsy sampling of much larger areas."
According to Zhongping Chen, associate professor of biomedical engineering at UCI's Beckman Laser Institute, the researchers have developed techniques that can show, in detail, blood flow through small vessels as well as microscopic changes in tissue.
"By coupling this imaging technology with a scanning microdevice that we can control with an endoscope, we may have arrived at an effective alternative to biopsy and visual screening for cancer," Chen said. "By inserting the tiny probe on the endoscope, we can perform imaging without cutting tissue and obtain results that are far better than what standard imaging can provide."
Miniature OCT
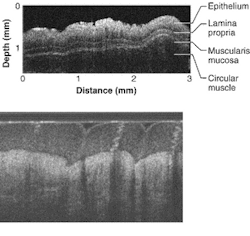
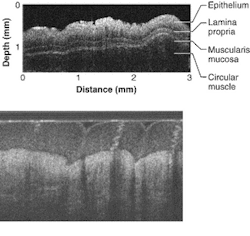
To view a tumor, the probe incorporates optical coherence tomography (OCT) to achieve high-speed surgical guidance at micron-scale resolution. Unlike conventional histopathology, the cross-sectional imaging technique does not require removal of tissue specimens for microscopic examination. Imaging with OCT eliminates the risks and sampling errors of excisional biopsy while providing image resolutions that are one to two orders above conventional ultrasound, creating a visual impression of tissue structure and blood flow with a sharpness not possible using other scanning methods.
While the penetration of OCT imaging in nontransparent tissue is only a few millimeters, the typical image resolution of OCT is 10 to 15 µm, 10 to 15 times greater than ultrasound, magnetic-resonance imaging, or computed tomography. Imaging with OCT is possible to resolutions as high as 1 to 10 µm. In addition, OCT is easy to interface to surgical microscopes, endoscopes, laparoscopes, catheters, and handheld probes without the need for active transducers and can be engineered into a compact, portable, and relatively inexpensive instrument. This makes OCT appropriate for surgical guidance and in vivo imaging in the gastrointestinal tract of animals and humans.
Chen, Chang, and their colleagues are now focusing on creating techniques for high-speed, high-resolution imaging on a scanner, a microscopic mechanical probe from silicon, and probes from plastic polymers and instituting clinical trials to test the capabilities of the imaging and mechanical probes in humans.