Femtosecond-laser tooth ablation promises less pain
A visit to the dentist’s chair is no one’s favorite outing. This reality will change only when tooth treatment becomes less unpleasant-which, despite modern turbine drilling, has not yet happened. Now, a laser-based tooth treatment developed by researchers at the University of Heidelberg’s Klinikum Mannheim (Mannheim, Germany) in cooperation with others in Germany and Austria promises not only a pain-free but also a reasonably economical treatment. In the technique, a highly precise form of tooth excavation, achieved by femtosecond-laser ablation, is at the same time an optimal preparation for subsequent tooth-repair work such as installing crowns.1
Tooth-tissue ablation has been explored using holmium:YAG and erbium:YAG lasers, excimer lasers, and others. The results, however, have been unimpressive, as a result of thermal side effects and long processing times. Using ultrafast laser pulses for this application was first proposed by one of the researchers (M. H. Niemz) in 1993. Ultrafast-laser/tissue interaction with high peak intensity favors a rapid plasma formation and, consequently, the transformation of the deposited energy into material ionization and ejection rather than heat transfer to the environment, so that side effects such as cracks and heat conduction to the nerves are greatly reduced. Pico- and femtosecond lasers have successfully been used.
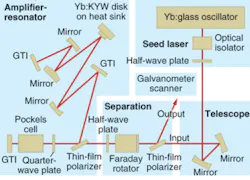
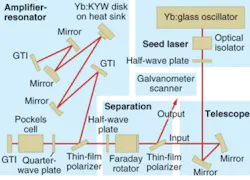
In their recent work, the researchers generated femtosecond-laser pulses by a straightforward approach without chirped-pulse amplification (CPA). Widely used in femtosecond-laser technology to prevent high-peak-power damage to optical components, CPA requires careful adjustment of optical components; such systems are suitable for research purposes but not for use in a dentist’s office. In the new technique, CPA is replaced by regenerative pulse amplification with intrinsic compensation of group velocity dispersion (see Fig. 1).
Femtosecond laser
A commercial ytterbium:glass laser tunable from 1030 to 1050‑nm and emitting 300-fs pulses was used as the seed laser. The 1-nJ output pulses were fed via an optical isolator (to avoid optical feedback) and a beam-expanding telescope to a separation unit that consisted of a thin-film polarizer, a Faraday rotator, and a half-wave plate, all for outcoupling the radiation returning from the amplifier.
Designed to produce a TEM00 (fundamental) mode, the amplifier resonator exhibited a beam quality M2 of 1.2. The amplification was achieved in a thin-disk (100-µm) 10%-ytterbium-doped potassium yttrium tungstate crystal mounted on a heat sink and optically pumped by a fiber-coupled diode laser in 16 passages of the pump beam. In the amplifier, two Gires-Tournois interferometer mirrors allowed for compensation of group-velocity dispersion. The injected seed pulse was captured for amplification over a multitude of roundtrips until being released, controlled by polarization switching using a beta barium borate Pockels cell. In this way, output pulses of up to 160 µJ and durations below 900 fs could be obtained at a repetition rate of 35 kHz. The beam was coupled out to a mirror that scanned the beam across the area to be ablated with a focal spot of 70 µm diameter.
Extracted human molar teeth were treated within one week after extraction (see Fig. 2). After extraction they had been stored in water to avoid dehydration. The maximum depth of the laser-ablated hole was about 0.5‑mm. The total processing time amounted to only a minute or so. Not only was the excavation precise, but a regular surface structure caused by the stepwise scanning of the laser pulses pointed to the potential for creating a roughened structure on the tooth surface that boosts adhesion required in later tooth repair.
The researchers found that carious tissue is ablated about ten times faster than sound tissue; this selectivity would cause the dentist to observe a dramatic slowdown of ablation speed when sound tissue is reached. The researchers expect processing times comparable to that of turbine drilling, as well as an almost pain-free treatment. The technique will be tested on human subjects in the near future.
REFERENCE
1. M. H. Niemz et al., Appl. Phys. B 79, 269 (2004).