Medical Lasers: Carbon monoxide laser shows surgical potential
Carbon monoxide (CO) and carbon dioxide (CO2) lasers are somewhat similar mid-infrared sources with very different histories. CO2 lasers have successfully serviced numerous industrial and medical applications over the past 50 years. But until recently, CO lasers were largely restricted to laboratory applications because of their limited reliability and lifetime, and their need for cryogenic cooling. However, in 2015, engineers at Coherent (Santa Clara, CA) solved issues of CO laser reliability and developed a family of sealed CO lasers that operate at room temperature, with lifetimes in the thousands-of-hours range.
The CO laser emits a cascade of wavelengths around 5.5 μm, which is about half the primary wavelength of the CO2 laser (at 10.6 μm). Many materials, including glass, water, and mammalian tissues, have very different absorption characteristics at these shorter wavelengths. Applications scientists at Art Photonics (Berlin, Germany) have recently been investigating how this difference in absorption manifests in laser-tissue interactions using one of the new Coherent lasers. This is a first step towards investigating the potential of these CO lasers as differentiated tools for surgical and related medical applications.
Many laser-surgery and other medical applications require fiber delivery. As explained by Viacheslav Artyushenko, president of Art Photonics, the company provides fiber light-delivery configurations from the ultraviolet through infrared, including the difficult 4-16 μm region, within which flexible cables are used that are based on polycrystalline infrared fibers (PIRs) extruded from silver halide crystals.
"Preliminary work in the past with an experimental CO laser indicated that its shorter wavelength could be an advantage in some surgical applications, because in some instances the shorter wavelength may provide up to two to three times deeper penetration than the CO2 laser," Artyushenko says. "We wanted to explore this further."
Matthias Schulze, director of marketing at Coherent, notes that the company wanted to investigate the surgical potential of the CO laser and thus provided a 40 W CO laser (C-55L-5) to conduct more-detailed studies.
Experimental comparison
The team compared the cuts made in several different animal tissue samples (heart, muscle, and liver) using a CO2 laser and the new CO laser. Cutting conditions were designed to be nearly identical for the two lasers, with a 0.5-mm-diameter laser output spot focused at a 2 mm depth within the tissue, and with the power level adjusted to 8 W. The different tissue samples were mounted on a translation stage under the fixed optics, enabling comparison of several cutting speeds (1, 2, and 4 mm/s). After cutting, the samples were frozen and cut with a scalpel perpendicular to the laser-cut direction. This enabled cross-sectional imaging of the laser cuts for qualitative and quantitative differences.
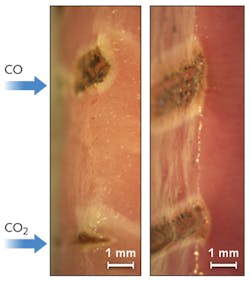
In all three tissue types and at every cutting speed, the Art Photonics team noticed significant differences in the results from the two laser wavelengths. The figure shows some typical results from the fatty muscle and heart muscle tissue samples.
"With laser tissue cutting, the two important parameters that are relatively easy to observe are how much tissue is ablated and the extent of the surrounding whiter zone, where the tissue is heated to its coagulation point but not removed," Artyushenko says. "In every case, we found that the CO2 laser produced deeper, narrower cuts, whereas the CO laser resulted in a wider and deeper coagulation zone. This is very exciting because coagulation is key to minimizing bleeding during laser surgery. However, we must remember that these experimental tests were made with dead tissue samples. The real comparison must be done in the future on tissue in vivo—when blood is running through the vessels and laser radiation should help to prevent bleeding during the laser cut."
Artyushenko notes that he has some historical evidence that low-power CO laser beams can successfully coagulate and cut a 2-mm-diameter rabbit artery in vivo with no bleeding.
The CO laser's superior coagulation capability could make it particularly well suited for surgery of highly vascularized tissues, where the risk of excessive bleeding might preclude the use of CO2 or solid-state (for example, erbium) lasers, Artyushenko adds. He cites examples such as welding of vessels, plastic surgery, and organ transplantation.
About the Author
John Wallace
Senior Technical Editor (1998-2022)
John Wallace was with Laser Focus World for nearly 25 years, retiring in late June 2022. He obtained a bachelor's degree in mechanical engineering and physics at Rutgers University and a master's in optical engineering at the University of Rochester. Before becoming an editor, John worked as an engineer at RCA, Exxon, Eastman Kodak, and GCA Corporation.
