Optical Coherence Tomography: OCTA clears quantitation hurdle
Optical coherence tomography angiography (OCTA) has achieved another milestone: mainstreaming of quantification—which Jay Wei, founder and CEO of OCTA instrumentation developer Optovue (Fremont, CA), calls “the gateway to widespread and global adoption of OCTA.”
The industry’s first OCTA blood-vessel-measurement technology—Optovue’s AngioAnalytics—won U.S. FDA 510(k) clearance in June 2018, three years after the FDA cleared the foundational OCTA technique for ophthalmology. The newly approved technology provides objective measurement of treatment efficacy for progressive sight-robbing diseases, and thereby promises “truly customized patient management and improved patient care,” Wei says.
OCTA is a high-resolution functional imaging technique that promises to impact ophthalmology as dramatically in the coming decade as OCT changed the field over the past decade.1 But without quantitation, its data are open to interpretation.
Objectivity, analysis, artifact removal
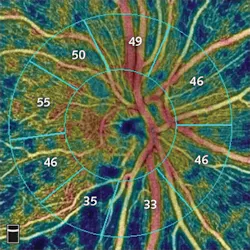
AngioAnalytics adds objective data and analysis to OCTA data produced by Optovue’s AngioVue instrument. Together, the hardware and software create color-coded maps of vessel densities in the retina or optic nerve, and analyses of areas of blood-vessel loss (nonperfusion), abnormal blood-vessel growth (flow area), and several parameters to assess change to the foveal avascular zone, an area of the retina profoundly affected by diabetic retinopathy (see figure). AngioAnalytics software also provides trend analysis, allowing physicians to objectively monitor retinal and vascular changes caused by disease progression or from treatment.
The company’s three-dimensional (3D) projection artifact removal software, 3D PAR, also received FDA clearance, promising greater enhancement of outcomes. Projection artifacts, inherent in all OCTA technology, occur when ghost images of blood vessels that exist in one retinal layer are projected onto other layers. These shadows hamper accurate interpretation of whether, and how much, abnormal vessel growth is actually present in the specific layers. Thus, 3D PAR technology forms the basis for accurate qualitative image interpretation and reliable measurements.
Paul E. Tornambe, MD, FACS, with Retinal Consultants of San Diego, CA, calls these software capabilities a game-changer because they render overlying inner retinal blood-vessel artifacts transparent, thus “allowing for better visualization and more accurate measurement of the outer retina and choroidal structures, essential in treating the abnormal blood-vessel growth (CNV membrane) that leads to blindness for patients with wet age-related macular degeneration (AMD),” he explains. He suggests that the technology provides a means of documenting the effect of drug treatment on “a specific CNV membrane in a specific patient, and how long that effect lasts,” thus enabling a means to monitor therapy or determine the need for additional treatment.
OCTA: high res, 3D, functional
Producers of the OCT Angiography Summit 2018 (Portland, OR; August 3-4), which explores technology advances and emerging clinical applications, call OCTA a “no-injection method of visualizing ocular circulation in three dimensions.” It’s a huge advance over the 2D imaging ophthalmologists have traditionally relied on to determine whether fluid is leaking from abnormal vessels in the retina, and whether additional treatment with VEGF inhibitor drugs would be helpful, Tornambe says.
A 2018 special issue of Case Reports in Ophthalmological Medicine, focused on OCTA, provides case reports that collectively illustrate many applications in patients with retinal and choroidal vascular diseases, as well as ocular oncology—applications for which it is currently best established.2 The role of OCTA is emerging for other macular and retinal diseases (including uveitis) and for glaucoma as well as optic nerve diseases.2
Complementary to traditional modalities such as fundus photography, fluorescein angiography (FA), and spectral-domain OCT (SD-OCT), label-free OCTA’s advantages include visualization of vascular flow signal, en face imaging, and segmentation of posterior segment structures in the eye.2 At the moment, OCTA also has some disadvantages, namely greater costs and acquisition times compared with SD-OCT, the latter of which can limit its ability to produce high-quality images in eyes with poor visual acuity that cannot fixate well.
Hot topics at the 2018 OCT Angiography Summit include OCTA’s role in glaucoma assessment, detection of choroidal neovascularization prior to leakage, and use of projection-resolved OCTA with adaptive optics to understand the retina’s vascular anatomy.
REFERENCES
1. A. H. Kashani et al., Prog. Retin. Eye Res., 60, 66–100 (2017).
2. S. G. Schwartz et al., Case Rep. Ophthalmol. Med., 7140164 (2018); https://doi.org/10.1155/2018/7140164.
About the Author

Barbara Gefvert
Editor-in-Chief, BioOptics World (2008-2020)
Barbara G. Gefvert has been a science and technology editor and writer since 1987, and served as editor in chief on multiple publications, including Sensors magazine for nearly a decade.