Spectroscopy techniques assist in revealing how potential HIV drug destroys the virus
Building on 15 years of work, a team of researchers from the Massachusetts Institute of Technology (MIT; Cambridge, MA) used advanced spectroscopy techniques to help them determine the mechanism behind the action of the HIV drug they developed, which they believe could help them develop better versions that would destroy the virus more quickly.
Related: Cytometry goes portable for HIV monitoring in remote areas
This type of drug could help combat the residual virus that remains in the T cells of patients whose disease has been brought into long-term remission by the triple-drug combination typically used to treat HIV, the researchers say. These viruses re-emerge periodically, which is why patients must stay on the drug cocktail indefinitely and are not considered "cured."
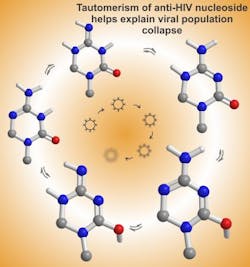
In the new study, the researchers discovered exactly how the drug, known as KP1212, induces the HIV genome to mutate. They used advanced spectroscopy techniques to analyze KP1212’s ability to promote tautomerism, a chemical phenomenon that involves the migration of protons among the nitrogen and oxygen atoms on nucleic-acid bases. This allowed the researchers to see that once KP1212 inserts itself into the genome, it can switch among five different shapes, or tautomers. Some of these behave like cytosine by pairing with guanine. However, some of the tautomers resemble thymine, so they will pair with adenine, introducing mutations.
"The five molecules are changing shape on a nanosecond timescale, and each shape has a different base-pairing property, so you will see a promiscuity in terms of the bases with which KP1212 pairs," says Vipender Singh, an MIT postdoc who was one of the study's lead authors.
To see this shape-shifting, the researchers used nuclear magnetic resonance (NMR) and a form of 2D infrared spectroscopy developed by Andrei Tokmakoff, a former MIT professor who is now at the University of Chicago and was one of the paper's senior authors, along with MIT professor John Essigmann. This technology allows scientists to determine the atomic composition and structure of nucleic-acid bases.
Then, using a genetic tool developed in the Essigmann lab, the researchers determined that KP1212 induces a mutation rate of exactly 10 percent in the HIV genome. Based on these findings, Essigmann estimates that if KP1212 doubles the mutation rate of HIV, it could clear the virus from patients in one to two years.
Essigmann says that Koronis Pharmaceuticals, the company they formed to develop the drug, hopes to run a longer trial of KP1212 and is also interested in developing drugs that would work faster, which could be accomplished by altering some of the chemical features of the molecule and testing whether they speed up the mutation rate.
The research team also hopes that the findings from their study could lead to future drug developments for dengue and yellow fevers.
Ribavirin, a drug used to treat hepatitis C, and the influenza drug T-705 are also believed to provoke hypermutation in their target viruses. The MIT team also plans to work with Lawrence Loeb, a professor of biochemistry at the University of Washington, to test the possibility of using similar compounds to force tumor cells to mutate themselves into extinction.
Full details of the work appear in the Proceedings of the National Academy of Sciences (PNAS); for more information, please visit http://dx.doi.org/10.1073/pnas.1405635111.
-----
Don't miss Strategies in Biophotonics, a conference and exhibition dedicated to development and commercialization of bio-optics and biophotonics technologies!
Follow us on Twitter, 'like' us on Facebook, and join our group on LinkedIn
Subscribe now to BioOptics World magazine; it's free!