OCT shows promise for faster detection of pneumonia-related bacteria in the ICU
A team of researchers at the University of California Irvine, the Beckman Laser Institute (both in Irvine, CA), and N8 Medical (Columbus, OH) demonstrated that optical coherence tomography (OCT) can be used to better detect and assess biofilm linked to a form of pneumonia prevalent in hospital intensive care units (ICUs).
Related Article
Biofilm has been connected to ventilator-associated pneumonia (VAP), which is a prevalent infection in hospital ICUs. Using OCT, the team was able to visualize and assess the extent of airway obstruction from biofilm deposited on intubated endotracheal tubes in vivo.
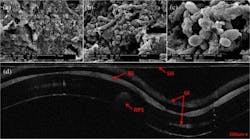
The current method for biofilm characterization utilizes scanning electron microscopy (SEM), a lengthy process that requires extracting a sample, drying it, and coating it with a thin gold layer, none of which can be performed in vivo. OCT, on the other hand, is a noninvasive imaging technology that can provide high-resolution, cross-sectional images of various biological samples, and can be adapted to provide 3D volumetric information.
In the research team's study, led by researcher Andrew Heidari, they extubated patients' endotracheal tubes and imaged them using both OCT and SEM. Biofilm was present in both images, and the researchers were able to use the OCT image to measure a reduction in endotracheal inner lumen area between a one-day intubation sample tube and a five-day sample tube. The study showed that OCT can be used to both detect the presence of biofilm and gather further information about the extent of biofilm formation from the thickness of biofilm observed.
In the future, the research group plans to use OCT images to analyze the thickness and structure of the biofilm at which intubated patients in the ICU contract VAP.
Full details of the work appear in the Journal of Biomedical Optics; for more information, please visit http://dx.doi.org/10.1117/1.JBO.20.12.126010.