Understanding cancer’s genetic makeup could halt its spread
Cells surrounding a tumor may hold the key to controlling the spread of breast cancer—but imaging those cells in finer detail and better understanding their genetic makeup could make all the difference. Now, researchers have found a way to do it.
The team, led by the Wellcome Trust Sanger Institute (U.K.)—alongside the European Molecular Biology Laboratory’s European Bioinformatics Institute (EMBL-EBI), the German Cancer Research Center, and the Science for Life Laboratory (Sweden)—has developed a technique to examine strands of cellular DNA and RNA with hundreds of thousands of small fluorescent molecular probes using fluorescence microscopy to scan much larger areas of tissue (see video).
Cell mutations, influenced in part by activity around the cells, often prompt breast cancer to grow uncontrollably, says Artem Lomakin, first author of the research who is a postdoctoral fellow at EMBL-EBI and a visiting researcher at the German Cancer Research Center. Breast cancer tumors eventually expand into cell clones and develop different mutations because they are genetically different and have varied reactions to treatment.
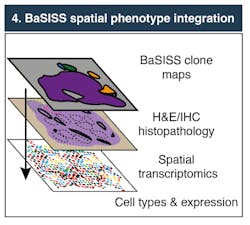
The new technique also incorporates a genetic clone mapping workflow grounded in base-specific in situ sequencing (BaSISS) technology, which aided the creation of quantitative maps of multiple genetic clones in eight tissues from two multifocal breast cancers, spanning the main histological stages of early breast cancer progression: ductal carcinoma in situ, invasive cancer, and lymph node metastasis (see Fig. 1). Researchers were able to monitor and identify changes in gene expression, and how they interact with the surrounding environment (see Fig. 2).“We want to read the genotypes of cells, preserving the spatial information. For all of the cells on a slide, we want to know what the genetic background is,” Lomakin says. “It's very complicated because generally there are very few DNA strands, usually two copies per cell. That’s a very, very low concentration, so it's particularly difficult.”
He notes that there are “a lot of tricks” the team has had to perform to amplify the signals detected, including developing the probe to target very specific mutations. This involved first determining exactly where in the tumor sample to survey—they could then hold and sequence several points along the sample.
“In this way, you will get enough resolution because you have bulk sequencing,” Lomakin says. “You will have enough resolution to find out what variants exist, and what mutations are attributable to different kinds of evolutionary lineages.”
The probes his team designed are usable on alleles, which are slightly different versions of the same genes created by mutations. The new method can provide information about the leading status of genes within cells. Using a process called rolling circle amplification—where a short DNA or RNA primer is amplified to form a long single-stranded DNA or RNA using a circular DNA template and special DNA or RNA polymerases—provides researchers a clearer, more enhanced view of the sample area. It produces “a very, very densely packed DNA strand that has a lot of copies,” Lomakin says.
“We can now target specific mutations in specific cells because usually when genes are expressed, there are multiple copies per cell,” he says. “When the gene is expressed from the DNA, it will also carry the mutation that was in the DNA on the original level.”
The researchers are now continuing the study, further exploring the internal and environmental markers that separate dangerous cancer evolutionary lineages from those that are more benign. They could also expand the cancer research into anything that has a cell structure internally.
“This technology will give us the ability to finally have the comprehensive picture of cancer evolution,” he says. “Historically, studies were done either in bulk or in single-cell levels. You lose spatial resolution in those cases, so you don't know which cells actually cooperate with each other. A technology like ours will be essential to understanding how cancer progresses.”
The research could also lead to development of therapies to slow or even prevent cancer cells’ ability to grow and spread by influencing the areas around a tumor.
About the Author
Justine Murphy
Multimedia Director, Digital Infrastructure
Justine Murphy is the multimedia director for Endeavor Business Media's Digital Infrastructure Group. She is a multiple award-winning writer and editor with more 20 years of experience in newspaper publishing as well as public relations, marketing, and communications. For nearly 10 years, she has covered all facets of the optics and photonics industry as an editor, writer, web news anchor, and podcast host for an internationally reaching magazine publishing company. Her work has earned accolades from the New England Press Association as well as the SIIA/Jesse H. Neal Awards. She received a B.A. from the Massachusetts College of Liberal Arts.