Imaging needle creates more complete picture for cancer care
Separately, different optical imaging tools can typically tell only part of a biomedical story. But a new technology from a team led by the University of Adelaide (Australia) could help tell a more complete tale.
“Optical imaging technologies are extremely useful for medicine, but they have some significant limitations,” says Robert McLaughlin, an Adelaide professor who is also the school’s chair of Biophotonics and leader of its Bioengineering Imaging Group. He cites shallow depth of light penetration in the body among the drawbacks.
Working together with optics engineers, chemists, and surgeons from throughout Australia and the U.K., he and fellow researchers from the University of Adelaide are addressing that and other limitations with a tiny probe that captures different types of images simultaneously.
The new probe consists of a highly miniaturized lens attached to the end of an optical fiber—both the lens and the fiber are about 125 µm in diameter.
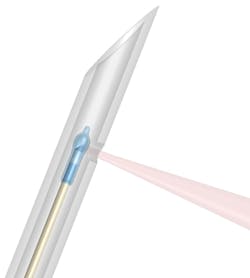
In the study, which is published in the Journal of Biomedical Optics, this tiny fiber-optic imaging probe was encased inside a stainless-steel needle with an outer diameter of 570 µm (see Fig. 1). “This is about the same size needle as would have been used the last time you received a vaccination,” McLaughlin says. “This allows us to insert the imaging probe deep into tissue without causing damage.”
Light is shone through the fiber to illuminate the tissue; at the same time, the light is collected through that same fiber (see Fig. 2). The new imaging probe—called a multimode imaging needle—can acquire two types of images: optical coherence tomography (OCT) and fluorescent.“We showed that an imaging probe small enough to fit inside a small needle is still sensitive enough to detect OCT and fluorescence signals from live tissue,” McLaughlin says.
For the OCT images, the researchers shine near-IR light on the tissue to detect light that is reflected from different depths within it, which ultimately creates an image of the overall tissue structure. This is conceptually similar to ultrasound, McLaughlin notes, but uses light waves instead of sound waves. It allows the researchers to achieve an image resolution of approximately 10 to 20 µm, as well as views of the shape and size of the groups of cells in the tissue.
Enhanced tissue differentiation
OCT alone is great for understanding tissue structure, but it may not differentiate between different types of tissue. With the new multimode imaging needle, the researchers “may be able to give the doctor a more complete understanding of what they are looking at,” he says.
To acquire the fluorescence images, the multimode imaging needle shines one wavelength of light and can then detect the light emitted from a different wavelength. Through fluorescent imaging, McLaughlin says the team can distinguish between types of tissue that otherwise appear very similar.
The researchers have also developed a fluorescent dye, which can precisely mark certain types of cancer cells. They created a fluorescent version of Tamoxifen, a common cancer drug, and used it to mark a subset of various breast cancer cells.
One major challenge in cancer-related surgeries is making sure all of the cancerous tissue has been removed. This is particularly common with breast cancer surgery, McLaughlin says, as it can be very difficult to identify small traces of cancerous tissue during the procedure.
“Our goal is to develop imaging tools that help surgeons perform more successful surgeries,” he says. “This research is a step toward developing tools that enable intra-operative image guidance to see these small traces of residual cancer.”
About the Author
Justine Murphy
Multimedia Director, Digital Infrastructure
Justine Murphy is the multimedia director for Endeavor Business Media's Digital Infrastructure Group. She is a multiple award-winning writer and editor with more 20 years of experience in newspaper publishing as well as public relations, marketing, and communications. For nearly 10 years, she has covered all facets of the optics and photonics industry as an editor, writer, web news anchor, and podcast host for an internationally reaching magazine publishing company. Her work has earned accolades from the New England Press Association as well as the SIIA/Jesse H. Neal Awards. She received a B.A. from the Massachusetts College of Liberal Arts.